One Health Investigation into Fatal Encephalitis Caused by Pigeon Paramyxovirus Type 1, France
Nicolas Veyrenche, Susana Boluda
1, Philippe Pérot
1, Isabelle Malissin, Marianne Leruez-Ville, Anne Jamet, Agnès Ferroni, Béatrice Regnault, Maud Salmona, Linda Feghoul, Laurine Robert-Capraro, Aurélie Leroux, Béatrice Grasland, Eric Niqueux, François-Xavier Briand, Isabelle Plu, Danielle Seilhean
2, Bruno Megarbane
2, Jacques Fourgeaud
2, and Nolwenn M. Dheilly
2
Author affiliation: Hôpital Necker-Enfants malades, Paris, France (N. Veyrenche, M. Leruez-Ville, A. Jamet, A. Ferroni, J. Fourgeaud); Université Paris Cité, FETUS, Paris (N. Veyrenche, M. Leruez-Ville, J. Fourgeaud); APHP-Hôpital de la Pitié-Salpêtrière, Sorbonne Université, Paris (S. Boluda, I. Plu, D. Seilhean); Institut Pasteur, Université de Paris, Paris (P. Pérot, B. Regnault, L. Robert-Capraro, N.M. Dheilly); Lariboisière Hospital, Paris Cité University, INSERM UMRS-1144, Paris (I. Malissin, L. Feghoul, B. Megarbane); Saint-Louis Hospital, APHP, Paris (M. Salmona); Biology and Pathogenesis of Viral Infection team, INSERM UMR 1342, Saint Louis Research Institute, Université Paris-Cité, Paris (M. Salmona); Anses, Ploufragan-Plouzané-Niort Laboratory, Ploufragan, France (A. Leroux, B. Grasland, E. Niqueux, F.-X. Briand)
Main Article
Figure 1
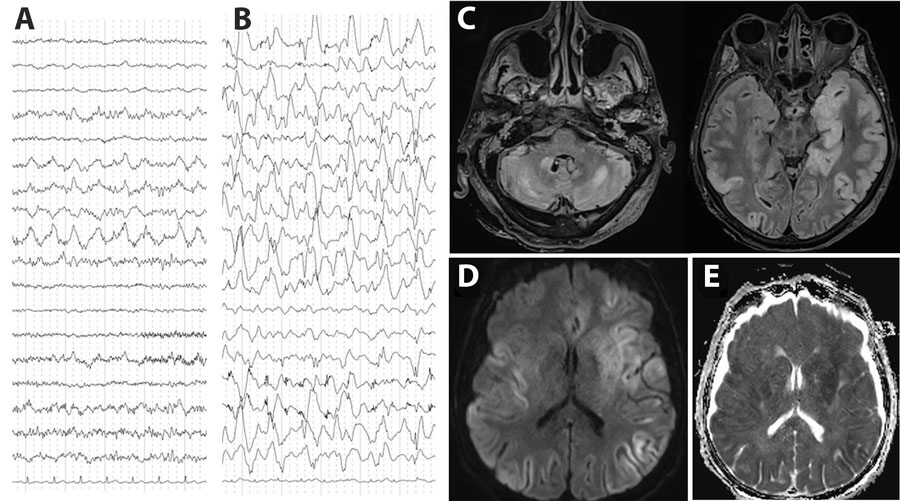
Figure 1. Electroencephalogram (EEG) and brain magnetic resonance imaging (MRI) testing of a patient with encephalitis caused by pigeon paramyxovirus type 1, France. A) The first EEG (day 5 after hospitalization) revealed nonspecific encephalopathy consisting of disorganized theta background rhythm and right temporal rhythmic delta focalization without seizure. B) A later EEG (day 23 after hospitalization) confirmed severe encephalitis with continuous, diffuse, nonreactive, high-amplitude, delta rhythm background of pseudo-periodic delta biphasic and triphasic waves, suggestive of cortical necrosis. C) MRI revealed diffuse bilateral fluid-attenuated inversion recovery hyperintensities, primarily cortical, with subcortical extensions, particularly to the temporal and insular regions, involving the pulvinar nuclei of the thalami, the basal ganglia, the internal capsule, the limbic system, and cerebellum. D, E) Hypersignals in diffusion-weighted images (D) and with reduced apparent diffusion coefficient (E) suggested diffuse cytotoxic brain edema in relation to severe necrotic encephalitis.
Main Article
Page created: March 31, 2026
Page updated: May 07, 2026
Page reviewed: May 07, 2026
The conclusions, findings, and opinions expressed by authors contributing to this journal do not necessarily reflect the official position of the U.S. Department of Health and Human Services, the Public Health Service, the Centers for Disease Control and Prevention, or the authors' affiliated institutions. Use of trade names is for identification only and does not imply endorsement by any of the groups named above.
