Volume 27, Number 1—January 2021
Dispatch
Coronavirus Disease among Workers in Food Processing, Food Manufacturing, and Agriculture Workplaces
Cite This Article
Citation for Media
Abstract
We describe coronavirus disease (COVID-19) among US food manufacturing and agriculture workers and provide updated information on meat and poultry processing workers. Among 742 food and agriculture workplaces in 30 states, 8,978 workers had confirmed COVID-19; 55 workers died. Racial and ethnic minority workers could be disproportionately affected by COVID-19.
High-density workplaces can cause high risk for transmission of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the virus that causes coronavirus disease (COVID-19) (1–3). US food processing, food manufacturing, and agriculture workplaces employ >3.6 million persons (4). Several factors contribute to workplace and community transmission, including prolonged close contact with coworkers, congregate housing, shared transportation, and frequent community contact among workers (1,2). Prior reports have characterized COVID-19 among meat and poultry processing workers (1,2). We describe COVID-19 among workers in other US food manufacturing and agriculture workplaces and update information on COVID-19 among meat and poultry processing workers.
The Centers for Disease Control and Prevention (CDC) collected cumulative aggregate data from state health departments on workers in US food processing, food manufacturing, and agriculture workplaces who had laboratory-confirmed COVID-19 (5). Requested data elements included the number and type of workplaces that reported >1 COVID-19 case among workers during March 1–May 31, 2020; the number of workers in affected workplaces; the number, demographics, and symptom status of workers with COVID-19; and the number of COVID-19–related deaths among workers. CDC requested the same information for meat and poultry processing workers and published preliminary data (1). Symptom data collection varied by workplace; clinical signs and symptom severity were not requested. None of these data had personal identifying information.
Workplaces were defined by the North American Industry Classification System codes 111 (Crop Production) and 311 (Food Manufacturing) (6). Demographic and symptom status proportions were calculated after excluding missing and unknown values. Data on sex were missing for 14.8% of food manufacturing and agriculture workers with COVID-19; on age for 13.4%; on symptom status for 33.6%; and on race and ethnicity for 36.3%. Because characteristics of total worker populations in affected workplaces were not available, we compared the racial and ethnic distribution of workers with COVID-19 to the distribution of all workers in the animal slaughtering and processing industry. CDC determined the investigation to be nonresearch as defined in 45 CFR 46.102(l); Paperwork Reduction Act was waived with respect to voluntary collection of information during a public health emergency (7).
Among 50 US states, 36 (72.0%) responded to the CDC inquiry; 33 (91.7%) reported >1 laboratory-confirmed COVID-19 case among food processing, food manufacturing, or agriculture workers during March 1–May 31, 2020. States reported 8,978 cases and 55 (0.6%) deaths among workers in 742 food manufacturing and agriculture workplaces in 30 states (Table 1). Among the 30 states reporting cases, the median number of affected facilities per state was 12 (interquartile range [IQR] 4–30 facilities); among 15 states that reported worker populations in affected workplaces, 8.2% of 30,609 workers received COVID-19 diagnoses. The percentage of workers with COVID-19 ranged from 2.0%–43.5% per state.
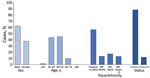
Of cases among food manufacturing and agriculture workers with information on sex (n = 7,647) and age (n = 7,771), 4,713 (61.6%) workers were male, 2,934 (38.4%) were female, and 3,439 (44.3%) workers were 20–39 years of age (Figure 1). Among 5,721 workers with race and ethnicity reported, 4,164 (72.8%) workers were Hispanic or Latino, 963 (16.8%) were non-Hispanic White, 362 (6.3%) were non-Hispanic Black, and 232 (4.1%) were non-Hispanic Asian/Pacific Islander. Overall, 83.2% of cases occurred among racial and ethnic minority workers. Symptom status was reported for 5,957 workers; 4,957 (83.2%) workers were symptomatic and 1,000 (16.8%) were asymptomatic or presymptomatic.
States reported 28,364 cases and 132 (0.5%) deaths among workers in 382 meat and poultry processing facilities in 31 states (Table 2). Demographic characteristics and symptom status of workers with COVID-19 indicated most were symptomatic and members of racial and ethnic minority groups (Figure 2).
We describe COVID-19 among workers in US food processing, food manufacturing, and agriculture workplaces during March 1–May 31, 2020. Among all food manufacturing and agriculture workers in 28 states reporting race and ethnicity data, 36.5% of workers are Hispanic or Latino, 52.6% are non-Hispanic White, 5.9% are non-Hispanic Black, 3.5% are non-Hispanic Asian/Pacific Islander, and 1.5% are of other non-Hispanic race or ethnicity groups (4). However, among workers with COVID-19 for whom race or ethnicity data were reported, 72.8% were Hispanic or Latino, 6.3% were non-Hispanic Black, and 4.1% were non-Hispanic Asian/Pacific Islander, suggesting that Hispanic or Latino, non-Hispanic Black, and non-Hispanic Asian/Pacific Islander workers in these workplaces might be disproportionately affected by COVID-19.
The sex, age, and symptom distribution of meat and poultry processing workers with COVID-19 was similar to that observed for food manufacturing and agriculture workers. The racial and ethnic distribution of meat and poultry processing workers with COVID-19 differed slightly; a higher percentage of cases were reported among non-Hispanic Black and non-Hispanic Asian/Pacific Islander workers.
Our study supports findings from prior reports that part of the disproportionate burden of COVID-19 among some racial and ethnic minority groups is likely related to occupational risk (8,9). These findings should be considered when implementing workplace interventions to ensure communication and training are culturally and linguistically tailored for each workforce.
Reports on mass testing in US meat and poultry processing facilities revealed widespread COVID-19 outbreaks and identified high proportions of asymptomatic or presymptomatic infections (10,11). Although most food manufacturing and agriculture workers (83.2%) and meat and poultry processing workers (88.1%) in our study reported symptoms, not all workplaces performed mass testing; therefore, workers with asymptomatic or presymptomatic infections might have been missed. These findings support the need for comprehensive testing strategies, coupled with contact tracing and symptom screening, for high-density critical infrastructure workplaces to aid in identifying infections and reducing transmission within the workplace (12).
Reducing workplace exposures is critical for protecting workers in US food processing, food manufacturing, and agriculture workplaces and might help reduce health disparities among disproportionately affected populations. Adherence to workplace-specific intervention and prevention efforts, including engineered controls, such as physical distancing; administrative controls, such as proper sanitation, cleaning, and disinfection; and providing personal protective equipment likely would protect both workers and surrounding communities (13,14).
This study has several limitations. First, only 36 states reported data; these results might not be representative of all US food processing, food manufacturing, and agriculture workers and workplaces. Second, testing strategies varied by workplace, influencing the number of cases detected and reported among workers. Workers might have been hesitant to report illness or seek healthcare, which could have led to underestimating cases among workers. Delays in linking cases and deaths to workplace outbreaks likely also contributed to an underestimation. Third, demographic characteristics of total worker populations in all affected workplaces were not available, limiting the ability to quantify the degree to which some racial and ethnic minority groups might be disproportionately affected by COVID-19. Fourth, preferred language, English proficiency, and migration and immigration status of workers were not captured; culturally and linguistically appropriate public health monitoring and interventions are crucial considerations for this workforce. Finally, workers are members of their local communities; transmission of SARS-CoV-2 could have occurred both at the workplace and in the surrounding community and thus could be affected by levels of community transmission.
Comprehensive evaluations in food processing, food manufacturing, and agriculture workplaces and communities are needed to clarify and address risk factors for SARS-CoV-2 transmission among workers. The extent of control measures and timing of implementations should be evaluated to assess effectiveness of workplace interventions. Several factors at the individual-, household-, community-, and occupational-level, including long-standing health and social disparities, likely contribute to disproportionate disease incidence among racial and ethnic minority workers.
Dr. Waltenburg is an Epidemic Intelligence Service Officer in the Division of Foodborne, Waterborne, and Environmental Diseases, National Center for Emerging and Zoonotic Infectious Diseases, CDC. Her primary research interests include epidemiology of and outbreak response for zoonotic diseases of public health importance.
Acknowledgments
We thank Logan Hudson, Ellie Morgan, Michelle Holshue, Alison Stargel, Alyssa Carlson, Laina Mitchell, Renee Canady, Tim Roth, Lea Hamner, Betsy Bertelsen, Anna Halloran, Sarah Murray, Zachary Doobovsky, Shawn Magee, Melissa Sixberry, Stephanie Kellner, Meredith Davis, Jonathan Richardson, Katrina Saphrey, Lisa Sollot, Julia Banks, Amal Patel, Betsy Schroeder, Alexander Neifert, Keith Amoroso, Lynn Bahta, Brooke Wiedinmyer, Mateo Frumholtz, Margaret Roddy, Paula Kriner, Jeff Lamoure, Linda Martinez, Karen Haught, Jessica Morales, Marifi Pulido, Lana O’Son, Alex U. Cox, and Jennifer Fuld for collating and collating epidemiologic data; Elyse Bevers and Jennifer Lam for data management support; Chas DeBolt and Laura Newman for conceptualization and consultation for Washington state; and Kristin Labar and Kate Fowlie for administrative support. We also thank the members of the CDC COVID-19 Emergency Response Team for their collaboration, including Michelle M. Dittrich, Gail Burns-Grant, Sooji Lee, Alisa Spieckerman, Kashif Iqbal, Sean M. Griffing, Alicia Lawson, Hugh M. Mainzer, Andreea E. Bealle, Erika Edding, Kathryn E. Arnold, Tomas Rodriquez, Sarah Merkle, Kristen Pettrone, Karen Schlanger, Alba E. Phippard, Kate Hendricks, Arielle Lasry, Vikram Krishnasamy, and Henry T. Walke.
T.K.H. Dostal is supported by the Applied Epidemiology Fellowship Program administered by the Council of State and Territorial Epidemiologists (CDC cooperative agreement no. 1NU38OT000297-01-00).
References
- Waltenburg MA, Victoroff T, Rose CE, Butterfield M, Jervis RH, Fedak KM, et al.; COVID-19 Response Team. COVID-19 Response Team. Update: COVID-19 among workers in meat and poultry processing facilities—United States, April–May 2020. MMWR Morb Mortal Wkly Rep. 2020;69:887–92. DOIPubMedGoogle Scholar
- Dyal JW, Grant MP, Broadwater K, Bjork A, Waltenburg MA, Gibbins JD, et al. COVID-19 among workers in meat and poultry processing facilities—19 States, April 2020. MMWR Morb Mortal Wkly Rep. 2020;69:557–61. DOIPubMedGoogle Scholar
- Baker MG, Peckham TK, Seixas NS. Estimating the burden of United States workers exposed to infection or disease: A key factor in containing risk of COVID-19 infection. PLoS One. 2020;15:
e0232452 . DOIPubMedGoogle Scholar - United States Census Bureau. 2014–2018 American community survey 5-year public use microdata samples (PUMS). 2018 [cited 2020 Jul 31]. https://www.census.gov/acs/www/data/data-tables-and-tools/data-profiles/2018
- Council of State and Territorial Epidemiologists. Coronavirus Disease 2019 (COVID-19) 2020 interim case definition. 2020 Apr 5 [cited 2020 May 26]. https://wwwn.cdc.gov/nndss/conditions/coronavirus-disease-2019-covid-19/case-definition/2020
- United States Census Bureau. North American industry classification system. 2017 [cited 2020 Jul 31]. https://www.census.gov/eos/www/naics
- United States Department of Health and Human Services, Office of the Assistant Secretary for Planning and Evaluation. Notice of Paperwork Reduction Act waiver – coronavirus disease 2019 (COVID-19). 2020 Apr 28 [cited 2020 May 24]. https://aspe.hhs.gov/system/files/pdf/258866/CDC-PHE-PRA-Waiver-Notice-COVID-19-04-28-20.pdf
- Hawkins D. Differential occupational risk for COVID-19 and other infection exposure according to race and ethnicity. Am J Ind Med. 2020;63:817–20. DOIPubMedGoogle Scholar
- Artiga S, Rae M. The COVID-19 outbreak and food production workers: who is at risk? 2020 Jun 3 Kaiser Family Foundation [cited 2020 Jul 31]. https://www.kff.org/coronavirus-covid-19/issue-brief/the-covid-19-outbreak-and-food-production-workers-who-is-at-risk
- Crews J. Tyson confirms hundreds of COVID-19 cases at Missouri chicken plant. Meat + Poultry. 2020 Jun 29 [cited 2020 Jul 31]. https://www.meatpoultry.com/articles/23379-tyson-confirms-hundreds-of-covid-19-cases-at-missouri-chicken-plant
- McCarthy R. Tyson announces more COVID-19 test results from Arkansas counties. Meat + Poultry. 2020 Jun 23 [cited 2020 Jul 31]. https://www.meatpoultry.com/articles/23340-tyson-announces-more-covid-19-test-results-from-arkansas-counties
- Centers for Disease Control and Prevention. Testing strategy for coronavirus (COVID-19) in high-density critical infrastructure workplaces after a COVID-19 case is identified. 2020 Jun 13 [cited 2020 Jul 31]. https://www.cdc.gov/coronavirus/2019-ncov/community/worker-safety-support/hd-testing.html
- Centers for Disease Control and Prevention. Meat and poultry processing workers and employers—interim guidance from CDC and the Occupational Safety and Health Administration (OSHA). 2020 Jul 9 [cited 2020 Aug 10]. https://www.cdc.gov/coronavirus/2019-ncov/community/organizations/meat-poultry-processing-workers-employers.html
- Centers for Disease Control and Prevention. Agriculture workers and employers—interim guidance from CDC and the U.S. Department of Labor. 2020 Jun 11 [cited 2020 Aug 10]. https://www.cdc.gov/coronavirus/2019-ncov/community/guidance-agricultural-workers.html
Figures
Tables
Cite This ArticleTable of Contents – Volume 27, Number 1—January 2021
| EID Search Options |
|---|
|
|
|
|
|
|

Please use the form below to submit correspondence to the authors or contact them at the following address:
Michelle Waltenburg, Centers for Disease Control and Prevention, 1600 Clifton Rd NE, Mailstop H24-10, Atlanta, GA 30329-4027, USA
Top