Volume 29, Number 3—March 2023
Research
COVID-19 Test Allocation Strategy to Mitigate SARS-CoV-2 Infections across School Districts
Cite This Article
Citation for Media
Abstract
In response to COVID-19, schools across the United States closed in early 2020; many did not fully reopen until late 2021. Although regular testing of asymptomatic students, teachers, and staff can reduce transmission risks, few school systems consistently used proactive testing to safeguard return to classrooms. Socioeconomically diverse public school districts might vary testing levels across campuses to ensure fair, effective use of limited resources. We describe a test allocation approach to reduce overall infections and disparities across school districts. Using a model of SARS-CoV-2 transmission in schools fit to data from a large metropolitan school district in Texas, we reduced incidence between the highest and lowest risk schools from a 5.6-fold difference under proportional test allocation to 1.8-fold difference under our optimized test allocation. This approach provides a roadmap to help school districts deploy proactive testing and mitigate risks of future SARS-CoV-2 variants and other pathogen threats.
By early January 2023, the COVID-19 pandemic had caused >6.7 million deaths worldwide (1), and severe socioeconomic hardship (2–4), particularly for racial minorities (5,6). Children experienced pandemic-related school closures, that led to substantial losses in learning (7–9), elevated rates of child abuse (10), lack of access to healthy food (11), and emotional harm (12). By the end of March 2020, all kindergarten through 12th grade (K–12) public schools in the United States had stopped in-person instruction (13), affecting 55 million students. Schools in 48 US states remained closed through the end of the school year (14). In August and September of 2020, a total of 74% of the 100 largest school districts in the United States started the year with remote-only teaching (15). By November 2020, 19% of those districts remained fully remote, and 36% had fully resumed in-person learning (15). Schools continued to reopen throughout the year.
By September 2021, a large fraction (70%) of US adults had been vaccinated with highly effective SARS-CoV-2 vaccines (16), including an estimated 86% of K–12 teachers and school staff (17). However, children <12 years of age were still ineligible for vaccines (16,18). Because large pockets of the country were still unvaccinated, COVID-19 continued to claim lives, and 100,000 deaths were reported in the United States during July–September 2021, including 246 deaths among children 0–17 years of age (16). At the end of October 2021, the United States authorized administration of COVID-19 vaccines for children 5–11 years of age (19). In January 2022, schools returned from winter break amidst a major COVID-19 wave fueled by the emergence of the highly transmissible and immune-evasive Omicron variant (F.P. Lyngse, unpub. data, https://doi.org/10.1101/2021.12.27.21268278), and case counts among students and staff reached record numbers despite increasing vaccine coverage in the United States (16,20).
Schools across the country adopted diverse reopening plans for the 2021–22 school year. Among the largest districts, 96% offered some form of in-person learning (21). Although some schools fully returned to prepandemic normal operations without COVID-19 interventions, many adopted policies for using, social distancing, quarantine, or testing requirements to safeguard the return to campus. The federal government invested $122 billion to support safe, in-person instruction through screening, improved building ventilation, purchase of personal protective equipment, hiring of additional personnel, and other measures (22,23). Within the first 2 months of the school year, ≈1.5% of schools closed temporarily in response to COVID-19 outbreaks (21).
Frequent and systematic testing of asymptomatic persons has been shown to be a viable and cost-effective mitigation strategy in communities, universities, and schools (24–29). However, tests are costly and inaccessible for many school districts in the United States; districts with limited testing resources must determine how to allocate testing across schools to protect their students, staff, and communities. Some districts have opted to restrict testing to symptomatic persons and other districts have apportioned tests according to school enrollment (30,31).
In this study, we propose a strategy for allocating testing resources across a diverse school district in which the frequency of testing depends on the school’s enrollment and grade range, recent COVID-19 cases reported among students and staff, and the estimated prevalence in the surrounding (i.e., catchment) community. Coupling derivative-free constrained optimization and a detailed agent-based simulation of SARS-CoV-2 transmission within and between classrooms, we derived an optimal allocation of tests across a school system that could minimize the maximum risk for cumulative infections on any campus over a 10-week period. We applied our approach to design a testing strategy for the 11 main high schools in the Austin Independent School District (AISD; Austin, Texas, USA), which has 18,500 enrolled students and 1,500 staff (32).
To determine an optimal allocation of tests across schools we developed a 2-step framework in which we first modeled COVID-19 transmission within schools for different levels of surveillance testing and then used those results as an input to an optimization model (Appendix). We first considered a hypothetical school system with 6 schools of 500 students each that differ over 2 parameters: community incidence and in-school transmission rate. For community incidence, we considered low and high scenarios. In the low scenario, the community had 35 new daily cases/100,000 persons; in the high scenario the community had 70 new daily cases/100,000 persons. For the transmission rate, we considered unmitigated R0 values to be low (1.0), moderate (1.5), or high (2.0).
We then modeled 11 high schools in AISD by using student enrollment based on attendance in early January 2021. We considered 2 different in-school transmission rate scenarios: an unmitigated transmission rate in all schools of with an R0 of 1.0; and transmission rates of each school estimated by fitting a regression model of the number of cases reported in that school against the estimated enrollment (33) (Appendix).
For each school and each scenario, we ran 300 stochastic simulations. We assumed that only students (not adult staff) were tested on Monday mornings and that test results were available instantly (34); preliminary analysis suggested that testing adults had minimal effects. During any given week, students in the model were selected for testing evenly across classes rather than testing a subset of entire classes.
In addition to proactive testing, we assumed that 90% of symptomatic persons would seek testing 0.5–1.5 days after symptom onset and then isolate after testing, even before results are available. We assumed 20% of infected students and 57% of infected adults would become symptomatic (35,36).
In our analysis of a hypothetical school system, we assumed that tests were perfectly accurate and that a positive test immediately triggered a 14-day isolation of the person and a 14-day quarantine of their household and classroom members. For our case study of AISD, we assumed lower test accuracy based on estimates for the widely used Abbott BinaxNow antigen tests (https://www.abbott.com), which had 95% sensitivity for symptomatic persons, 80% sensitivity for asymptomatic persons, and 99% specificity (37,38).
Transmission Model
We built a stochastic agent-based model of COVID-19 transmission within schools that included household transmission for students. We held the average community incidence constant through the simulation and all persons could become infected through outside interactions that were not explicitly modeled. The modeled population included students, teachers, staff, bus drivers, and members of the students’ households. We modeled various contacts between agents in schools (Appendix).
We used published estimates for the average SARS-CoV-2 incubation, latent, and infectious periods, as well as a person’s infectiousness through time (39). We assumed that asymptomatic cases were two thirds as infectious as symptomatic cases (40).
We simulated contacts at half-hour intervals and stochastically determined infection events based on the transmission probability between pairs of interacting persons. For each scenario, we derived the transmission rate to produce the specified unmitigated in-school R0 (Appendix). This R0 is the basic reproductive rate we would obtain without any testing, symptomatic or surveillance, and reflects other mitigation measures in place, such as face masks or social distancing.
We ran simulations for 10 weeks. We initiated simulations with everyone susceptible and simulated community and household infections for 10 days before school started.
Optimization Model
The objective of our test-allocation problem was to minimize the maximum risk experienced by any school in the system under consideration. Because of the stochastic nature of our COVID-19 transmission model, we had to choose a measure that summarized the risk for a given school under each possible frequency of surveillance testing. We defined the risk for each school as the expected number of on-campus infections of students plus the 90% conditional value-at-risk (CVaR) of the number of on-campus infections. Here, CVaR represents the expected number of such infections, conditional on restricting attention to the worst 10% of simulated outcomes, and hence accounts for risk aversion. Given 2 candidate allocations with a similar average number of cases, we preferred the allocation that limited the upside tail risk in terms of a large outbreak. We further accounted for risk by taking the worst-case risk measure across all schools. We used on-campus infections, rather than total infections, because total infections are partially driven by community incidence rather than school interventions. We further used the proportion of a school’s infected population rather than the absolute number of infections, which enabled us to treat large and small schools equally. Then, we could calculate each school’s risk as a function of the number of tests allocated; more tests reduced the risk incurred. Our goal was to allocate tests to schools to minimize the largest risk measure incurred at any school, subject to the constraints that we respect total testing capacity across the school system and that we cannot test all students at a school more than once per week (Appendix Figure 13).
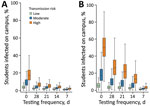
Under all transmission scenarios, we expected proactive testing to greatly reduce the proportion of students infected on campus over a 10-week period (Figure 1, panel A). In the high-risk scenario (in-school R0 = 2.0), 14-day testing reduced the fraction of students infected from 18.2% to 4.1%; under the lowest risk scenario (in-school R0 = 1.0), the expected incidence decreased from 4.0% to 1.5%. When we increased testing frequency from every 14 days to every 7 days, the expected incidence in high-risk scenario reduced to 2.1% and expected incidence in low-risk scenario reduced to 1.0%.
The efficacy of testing to mitigate in-school transmission depended on whether quarantine was limited to the household of the positive case or extended to the entire classroom (Figure 1, panel B). Under a moderate transmission scenario (in-school R0 = 1.5) in which students are tested every other week, the expected incidence decreased from 6.3% (95% CI 1.0%–15.6%) to 2.9% (95% CI 1.0%–6.2%) when we added classroom quarantine to household quarantine. We also estimated the costs of quarantine in terms of days of in-school education lost over the 10-week projection period, under the moderate transmission risk scenario (Figure 2, panel A; Appendix Figure 11). Without proactive testing, we expected the strategy of quarantining entire classrooms after a positive test to result in an average of 3 (6%) out of 50 school days missed per student. We expected household-only quarantine to reduce that cost by roughly 6.5-fold, to an average 0.9% of school days missed; however, that strategy roughly doubled the days students spent at school while infectious (Figure 2, panel B).
Regardless of quarantine policy, our model showed that proactive testing could reduce in-school exposure, with few to no additional lost days of school. In addition, we found that shortening the quarantine period for classroom contacts from 14 to 7 days would mitigate some of the educational losses without substantially increasing health risks (Appendix Figure 12).
As a sensitivity analysis, we also considered a higher rate of SARS-CoV-2 introductions from the surrounding community by raising daily new cases from 35 cases/100,000 persons to 70 cases/100,000 persons and lowering the accuracy of SARS-CoV-2 tests (37,38) (Appendix Figures 10, 11). In our sensitivity analysis, we found that our estimates were robust to the assumed sensitivity and specificity of the tests (Appendix).
Case Study—Optimizing Testing across a Large Municipal School District
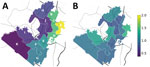
We applied our model to derive an optimal allocation of testing resources across the 11 high schools in AISD, the largest district in Austin, Texas, which includes 75,000 students, 5,500 teachers, and 5,000 staff. The district operates 125 schools from pre-K–12th grade; 55% of students are Hispanic and 30% White, and >50% come from economically disadvantaged backgrounds (32). We estimated the external force of infection for each school by comparing reported COVID-19 incidence in the neighborhood of a school to reported incidence across the entire metropolitan statistical area (MSA) from March 2020–January 2021 (Figure 3, panel A) (41). We listed the schools in order of the estimated external risks; the catchment of school A had almost double (195%) the city-wide incidence, and the catchment of school K had only 37%. In general, risk (i.e., COVID-19 incidence) was higher on the east side of Austin.
We estimated on-campus transmission risk for each school by using reported cases from each school during August 16, 2020–March 8, 2021 (Figure 3, panel B). In brief, we scaled the in-school R0 based on the difference between the cumulative, per student incidence in a school to the cumulative incidence throughout the district. We assumed a baseline R0 of 1.0; thus, schools with incidence equal to the district-wide incidence had resulting estimates that ranged from 0.70–1.41. Our estimates for on-campus transmission risk and external force of infection were not greatly correlated (Appendix). We also ran scenarios in which all schools had the same transmission risk (Appendix Figures 5, 6).
On the basis of the estimated heterogeneity in risks across the district, we estimated the optimal allocation of testing resources across schools by searching the space of possible allocations. For a given allocation, we projected the outcome for each school by first averaging the expected cumulative incidence (i.e., the mean across 300 simulations) and then the projected tail risk (i.e., the mean across the 10% worst-outcome simulations). We found the maximum value across schools (i.e., the projection for the highest-risk school) and then selected the allocation that minimized this value. Assuming that the average community incidence was 70 new daily cases per 100,000 population, based on estimates from late January 2021 in the Austin area (42), and that the district had a total testing budget of 1 test per student every 14 days across the district, the optimized allocation ranged from testing once per 45 days in the lowest-risk school (school K) to once per 7 days in the highest-risk school (school A) (Figure 4, panel A). We assumed that testing could not be administered more frequently than weekly. The optimal allocation differed slightly when we assumed instead that schools had the same on-campus R0 and differences in risk stemmed solely from the community force of infection (Figure 4, panel A).
We projected infection rates under both the optimized allocation and a nonoptimized pro rata allocation in which resources would be allocated proportional to enrollment (Figure 4, panel A). We expected the optimized strategy to slightly reduce the overall infection rate for the district relative to the pro rata strategy and equalize risks across campuses. In the optimized strategy, the median infection rate increased by 0.4% for the lowest-risk school (school K) and decreased by 1.8% for the highest-risk school (school A) (Appendix Table 4).
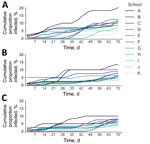
When we considered total incidence by combining both community-acquired and school-acquired infections, we expected ≈5.8-fold difference between the highest risk and lowest risk schools, in the absence of testing (Figure 5, panel A). Using a 14-day testing budget, we found a pro rata strategy would lower overall incidence but not reduce the disparity (Figure 5, panel B), but an optimized allocation would greatly shrink the gap to a 3.6-fold difference (Figure 5, panel C). Restricting our analysis to infections that occur on campus, the optimized allocation again reduced the disparity in risk across schools (Table).
To provide intuition, we also derived an optimal testing allocation to reduce risks in a hypothetical district containing 6 schools, 1 of each combination of either low or high external risk and either low, moderate, or high internal risk (Appendix Figures 8, 9). We compared 3 possible testing scenarios: no testing, universal testing every 2 weeks, and an optimal testing strategy in which the 2-week testing budget is allocated to schools to minimize the maximum risk experienced by any school in the system. We found that going from no testing to a pro rata allocation decreased the maximum risk for any school from 24.7% (95% CI 11.9–38.0) of students infected to 6.6% (95% CI 3.0–11.4); under the optimal allocation, risk was further reduced to 4.5% (95% CI 1.4–8.3). Using this strategy, the total expected risk across all 6 schools was reduced from 12.8% (95% CI 9.0–16.9) of infections without testing to 3.8% (95% CI 2.5–5.2) with a pro rata allocation, which was further reduced to 3.5% (95% CI 2.4–4.8) under the optimal testing allocation (Appendix Figure 14, panel B).
Proactive testing can be an effective strategy for preventing SARS-CoV-2 transmission on school campuses, if test turnaround is short and positive cases are immediately isolated (44; A. Bilinski, unpub. data, https://doi.org/10.1101/2021.05.12.21257131). Because testing requires considerable time, resources, and personnel, schools might opt to streamline their efforts as COVID-19 risks change. Our study provides a framework to help school districts allocate limited testing resources across different schools, depending on the in-school and local community transmission risks, while weighing the costs and benefits of classroom quarantine after a positive test. Prioritizing testing based on estimated risks can help mitigate the disproportionate COVID-19 burden falling on lower socioeconomic and racial minority neighborhoods (45–47).
Our results suggest that the optimal allocation of tests across schools depends on both the in-school transmission rate and the force of infection from the surrounding community. However, estimating in-school risks is difficult without sufficient testing because of overdispersion in the distribution of secondary cases and the small proportion of children that develop symptoms upon SARS-CoV-2 infection (48). A modest level of baseline surveillance testing could help determine the relative risks across schools (49). Our case study of AISD high schools suggests that even without such information, allocating testing resources based on community risks alone could substantially close gaps among schools (Appendix Figure 7).
Although proactive testing can lower and equalize COVID-19 risks across a heterogeneous school district, disparities are likely to persist. Schools drawing from neighborhoods with high COVID-19 incidence will continue to experience higher case counts and absenteeism. Other intervention measures, including vaccination and use of face masks, are essential for further reducing risks and ensuring equitable access to education.
The optimal allocation of scarce resources across multiple entities, like the number of tests per school, depends on the state of the entire system. A school might receive anywhere from no tests to enough tests for weekly testing of every student, depending on the level of risk relative to other schools. Schools could potentially game the system to gain larger allocations. For example, a school could inflate reported cases or enable higher rates of transmission by allowing high-risk activities or relaxing precautionary measures. If such issues arose, then allocation calculations could be based solely on estimates for the force of infection from the surrounding communities.
This approach can be broadly applied to distributing limited SARS-CoV-2 testing resources across systems with heterogeneous risks, such as workplaces, correctional facilities, or long-term care facilities. Our case study demonstrates that, even within a single city, tailoring control strategies to hyperlocal estimates of risks can reduce transmission overall and mitigate chronic disparities in access to resources and disease burden. On larger geographic scales, spatiotemporal variation in COVID-19 risks has been even more apparent, and cities, states, and countries exhibit highly asynchronous waves of transmission. Dynamic allocation of scarce public health resources based on reliable estimates of risk could substantially reduce the burden of COVID-19 and future pathogen threats across the United States but requires considerable coordination at the state and federal level.
The first limitation of our study is that we assumed immediate in-school and community risks could be reliably estimated. In practice, the data required to estimate such risks often lag, are biased, or are unavailable. Such uncertainty could be included in our model by using stochastic variables that evolve based on test results from each school. However, the additional complexity would slow computational optimization. Second, we estimated heterogeneity in incidence but did not explicitly consider vaccination, health outcomes other than incidence, or socioeconomic or other factors known to correlate with COVID-19 risks (50). Schools drawing from more vulnerable communities might have access to fewer mitigation resources besides testing, lower vaccination coverage, or higher infection hospitalization and mortality rates. Such factors could be explicitly modeled and incorporated into the objective function used to derive equitable allocations. Third, the study derived allocations to minimize infections occurring across a school district. However, other outcomes could be explicitly incorporated into further analyses, including absenteeism and loss of education resulting from isolation and quarantine. The costs and benefits of quarantining entire classrooms, in addition to the households of positive cases, depend on the frequency of testing. Classroom quarantine would always be expected to elevate absenteeism but only substantially reduces exposure risks when testing is infrequent. With frequent testing or low transmission risks, limiting the scope and duration of quarantine might be advisable. Hospitalization risks for school staff and the potential for schools to exacerbate transmission in the surrounding community also could be integrated into allocation calculations. Finally, our model does not consider the potential costs or logistical impediments to dynamically allocating tests among schools. In addition to the challenges of rapidly calculating allocations and distributing tests accordingly, schools might require additional trained staff to administer tests, conduct contact tracing, and ensure the quick and safe isolation and quarantine of affected persons (30).
In conclusion, as the United States plans for COVID-19 postpandemic management, proactive testing will remain a highly effective countermeasure that can be tailored to changing risks on a local scale. As tests become more economical and as surveillance within schools and communities improves, our model demonstrates that school systems can optimize testing and quarantine policies to prevent transmission, limit absenteeism, and ensure continuity of operations during future COVID-19 surges.
Mr. Pasco is a PhD candidate at the University of Texas at Austin, Austin, Texas, USA. His research interests include mathematical modeling of infectious diseases and operations research.
Acknowledgments
We thank the Texas Advanced Computing Center at The University of Texas (Austin, TX, USA) for providing high performance computing and database resources that contributed to the research results.
This work was supported by grant no. U01IP001136 from the Centers for Disease Control and Prevention, grant no. NIH-R01-AI151176 from the National Institutes of Health, grant no. 17STQAC00001-04-00US from the Department of Homeland Security, and a generous donation from Tito’s Handmade Vodka. The funders had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; or decision to submit the manuscript for publication. The views and conclusions contained in this document are those of the authors and should not be interpreted as necessarily representing the official policies, either expressed or implied, of the funding institutions.
References
- Johns Hopkins Coronavirus Resource Center. COVID-19 map [cited 2023 Jan 13]. https://coronavirus.jhu.edu/map.html
- United Nations Conference on Trade and Development. COVID-19’s economic fallout will long outlive the health crisis, report warns [cited 2021 Apr 13]. https://unctad.org/news/covid-19s-economic-fallout-will-long-outlive-health-crisis-report-warns
- Czeisler MÉ, Lane RI, Petrosky E, Wiley JF, Christensen A, Njai R, et al. Mental health, substance use, and suicidal ideation during the COVID-19 pandemic—United States, June 24–30, 2020. MMWR Morb Mortal Wkly Rep. 2020;69:1049–57. DOIPubMedGoogle Scholar
- Vahratian A, Blumberg SJ, Terlizzi EP, Schiller JS. Symptoms of anxiety or depressive disorder and use of mental health care among adults during the COVID-19 pandemic—United States, August 2020–February 2021. MMWR Morb Mortal Wkly Rep. 2021;70:490–4. DOIPubMedGoogle Scholar
- Center on Budget and Policy Priorities. Tracking the COVID-19 recession’s effects on food, housing, and employment hardships [cited 2021 Apr 13]. https://www.cbpp.org/research/poverty-and-inequality/tracking-the-covid-19-recessions-effects-on-food-housing-and
- Parker K, Minkin R, Bennett J. Economic fallout from COVID-19 continues to hit lower-income Americans the hardest. Pew Research Foundation; 2020 Sep 24 [cited 2021 Apr 13]. https://www.pewresearch.org/social-trends/2020/09/24/economic-fallout-from-covid-19-continues-to-hit-lower-income-americans-the-hardest
- Azevedo JP, Hasan A, Goldemberg D, Geven K, Iqbal SA. Simulating the potential impacts of COVID-19 school closures on schooling and learning outcomes: a set of global estimates [cited 2021 Apr 13]. World Bank Res Obs. 2021;36:1–40 https://academic.oup.com/wbro/article-pdf/36/1/1/36757308/lkab003.pdf.
- Engzell P, Frey A, Verhagen MD. Learning loss due to school closures during the COVID-19 pandemic. Proc Natl Acad Sci U S A. 2021;118:
e2022376118 . DOIPubMedGoogle Scholar - Dorn E, Hancock B, Sarakatsannis J, Viruleg E. COVID-19 and learning loss—disparities grow and students need help. McKinsey & Company. 2020 [cited 2021 Apr 13]. https://www.mckinsey.com/industries/public-and-social-sector/our-insights/covid-19-and-learning-loss-disparities-grow-and-students-need-help
- Baron EJ, Goldstein EG, Wallace CT. Suffering in silence: How COVID-19 school closures inhibit the reporting of child maltreatment. J Public Econ. 2020;190:
104258 . DOIPubMedGoogle Scholar - Kinsey EW, Hecht AA, Dunn CG, Levi R, Read MA, Smith C, et al. School closures during COVID-19: opportunities for innovation in meal service. Am J Public Health. 2020;110:1635–43. DOIPubMedGoogle Scholar
- Orgilés M, Morales A, Delvecchio E, Mazzeschi C, Espada JP. Immediate psychological effects of the COVID-19 quarantine in youth from Italy and Spain. Front Psychol. 2020;11:
579038 . DOIPubMedGoogle Scholar - Honein MA, Barrios LC, Brooks JT. Data and policy to guide opening schools safely to limit the spread of SARS-CoV-2 infection. JAMA. 2021;325:823–4. DOIPubMedGoogle Scholar
- Education Week Staff. A year of COVID-19: what it looked like for schools. Education Week. 2021 Mar 4 [cited 2021 Nov 2]. https://www.edweek.org/leadership/a-year-of-covid-19-what-it-looked-like-for-schools/2021/03
- Center for American Progress. Remote learning and school reopenings: what worked and what didn’t [cited 2021 Nov 2]. https://www.americanprogress.org/issues/education-k-12/reports/2021/07/06/501221/remote-learning-school-reopenings-worked-didnt
- US Centers for Disease Control and Prevention. COVID data tracker [cited 2021 Aug 12]. https://covid.cdc.gov/covid-data-tracker/#vaccinations_vacc-total-admin-rate-total
- Busser C. NEA survey finds educators back in classrooms and ready for fall. National Education Association. 2021 Jun 17 [cited 2021 Nov 2]. https://www.nea.org/about-nea/media-center/press-releases/nea-survey-finds-educators-back-classrooms-and-ready-fall
- Gutman-Wei R. Why is it taking so long to get vaccines for kids? The Atlantic. 2021 Aug 11 [cited 2021 Aug 12]. https://www.theatlantic.com/health/archive/2021/08/covid-vaccination-timeline-children/619729/
- US Food and Drug Administration. FDA Authorizes Pfizer-BioNTech COVID-19 vaccine for emergency use in children 5 through 11 years of age [cited 2021 Dec 6]. https://www.fda.gov/news-events/press-announcements/fda-authorizes-pfizer-biontech-covid-19-vaccine-emergency-use-children-5-through-11-years-age
- Goldstein D. Omicron upends return to school in U.S. The New York Times. 2022 Jan 3 [cited 2022 Jan 5]. https://www.nytimes.com/live/2022/01/03/us/school-closings-covid
- Parks SE, Zviedrite N, Budzyn SE, Panaggio MJ, Raible E, Papazian M, et al. COVID-19–related school closures and learning modality changes—United States, August 1–September 17, 2021. MMWR Morb Mortal Wkly Rep. 2021;70:1374–6. DOIPubMedGoogle Scholar
- US Department of Health and Human Services. Biden administration to invest more than $12 billion to expand COVID-19 testing [cited 2021 Jul 7]. https://www.hhs.gov/about/news/2021/03/17/biden-administration-invest-more-than-12-billion-expand-covid-19-testing.html
- US Department of Education. Department of Education announces American Rescue Plan funds for all 50 States, Puerto Rico, and the District of Columbia to help schools reopen [cited 2021 Jul 5]. https://www.ed.gov/news/press-releases/department-education-announces-american-rescue-plan-funds-all-50-states-puerto-rico-and-district-columbia-help-schools-reopen
- Larremore DB, Wilder B, Lester E, Shehata S, Burke JM, Hay JA, et al. Test sensitivity is secondary to frequency and turnaround time for COVID-19 screening. Sci Adv. 2021;7:
eabd5393 . DOIPubMedGoogle Scholar - Du Z, Pandey A, Bai Y, Fitzpatrick MC, Chinazzi M, Pastore Y Piontti A, et al. Comparative cost-effectiveness of SARS-CoV-2 testing strategies in the USA: a modelling study. Lancet Public Health. 2021;6:e184–91. DOIPubMedGoogle Scholar
- Paltiel AD, Zheng A, Walensky RP. Assessment of SARS-CoV-2 screening strategies to permit the safe reopening of college campuses in the United States. JAMA Netw Open. 2020;3:
e2016818 . DOIPubMedGoogle Scholar - Lanier WA, Babitz KD, Collingwood A, Graul MF, Dickson S, Cunningham L, et al. COVID-19 testing to sustain in-person instruction and extracurricular activities in high schools—Utah, November 2020–March 2021. MMWR Morb Mortal Wkly Rep. 2021;70:785–91. DOIPubMedGoogle Scholar
- Frazier PI, Cashore JM, Duan N, Henderson SG, Janmohamed A, Liu B, et al. Modeling for COVID-19 college reopening decisions: Cornell, a case study. Proc Natl Acad Sci U S A. 2022;119:
e2112532119 . DOIPubMedGoogle Scholar - Vohra D, Rowan P, Goyal R, Hotchkiss J, O’Neil S. Early insights and recommendations for implementing a covid-19 antigen testing program in K-12 schools: lessons learned from six pilot sites. New York: The Rockefeller Foundation; 2021 [cited 2021 Apr 13]. https://www.rockefellerfoundation.org/wp-content/uploads/2021/02/Early-Insights-and-Recommendations-for-K-12-Schools-Covid-19-Testing-Lessons-Learned-from-Six-Pilot-Sites.pdf
- Faherty LJ, Master BK, Steiner ED, Kaufman JH, Predmore Z, Stelitano L, et al. COVID-19 testing in K-12 schools–insights from early adopters. Santa Monica (CA): RAND Corporation; 2021 [cited 2021 Jul 5]. https://www.rockefellerfoundation.org/wp-content/uploads/2021/02/RAND_Covid-19-Testing-in-K-12-Schools_Insights-from-Early-Adopters.pdf
- Howard J. Debate emerges around Covid-19 testing strategies in schools as districts plan to reopen. CNN. 2021 Jul 19 [cited 2021 Nov 2]. https://www.cnn.com/videos/tv/2021/07/19/lead-erica-hill-live-jake-tapper.cnn
- Austin Independent School District. About our schools [cited 2021 May 19]. https://www.austinisd.org/schools
- Austin Independent School District. COVID-19 dashboard [cited 2021 Apr 14]. https://www.austinisd.org/openforlearning/dashboard
- Abbott. Taking COVID-19 testing to a new level [cited 2021 Apr 14]. https://www.abbott.com/BinaxNOW-Test-NAVICA-App.html
- Davies NG, Klepac P, Liu Y, Prem K, Jit M, Eggo RM; CMMID COVID-19 working group. Age-dependent effects in the transmission and control of COVID-19 epidemics. Nat Med. 2020;26:1205–11. DOIPubMedGoogle Scholar
- Gudbjartsson DF, Helgason A, Jonsson H, Magnusson OT, Melsted P, Norddahl GL, et al. Spread of SARS-CoV-2 in the Icelandic population. N Engl J Med. 2020;382:2302–15. DOIPubMedGoogle Scholar
- Pollock NR, Jacobs JR, Tran K, Cranston AE, Smith S, O’Kane CY, et al. Performance and implementation evaluation of the Abbott BinaxNOW Rapid Antigen Test in a high-throughput drive-through community testing site in Massachusetts. J Clin Microbiol. 2021;59:e00083–21. DOIPubMedGoogle Scholar
- US Food and Drug Administration. Abbott BinaxNOW COVID-19 Ag CARD instructions for use and characteristics [cited 2021 Apr 19]. https://www.fda.gov/media/141570/download
- He X, Lau EHY, Wu P, Deng X, Wang J, Hao X, et al. Temporal dynamics in viral shedding and transmissibility of COVID-19. Nat Med. 2020;26:672–5. DOIPubMedGoogle Scholar
- He D, Zhao S, Lin Q, Zhuang Z, Cao P, Wang MH, et al. The relative transmissibility of asymptomatic COVID-19 infections among close contacts. Int J Infect Dis. 2020;94:145–7. DOIPubMedGoogle Scholar
- University of Texas at Austin COVID-19 Modeling Consortium. Heterogeneous burden of the COVID-19 pandemic in central Texas [cited 2021 Apr 25]. https://sites.cns.utexas.edu/sites/default/files/cid/files/austin_covid-19_spatial_burden_report.pdf
- University of Texas at Austin COVID-19 Modeling Consortium. Austin dashboard [cited 2021 Nov 5]. https://covid-19.tacc.utexas.edu/dashboards/austin
- Liu Q-H, Zhang J, Peng C, Litvinova M, Huang S, Poletti P, et al. Model-based evaluation of alternative reactive class closure strategies against COVID-19. Nat Commun. 2022;13:322. DOIPubMedGoogle Scholar
- Rubin-Miller L, Alban C, Artiga S, Sullivan S. COVID-19 Racial Disparities in Testing, Infection, Hospitalization, and Death: Analysis of Epic Patient Data. Kaiser Family Foundation; 2020 Sep 15 [cited 2021 Jul 5]. https://www.kff.org/coronavirus-covid-19/issue-brief/covid-19-racial-disparities-testing-infection-hospitalization-death-analysis-epic-patient-data
- Mena GE, Martinez PP, Mahmud AS, Marquet PA, Buckee CO, Santillana M. Socioeconomic status determines COVID-19 incidence and related mortality in Santiago, Chile. Science. 2021;372:
eabg5298 . DOIPubMedGoogle Scholar - Martin CA, Jenkins DR, Minhas JS, Gray LJ, Tang J, Williams C, et al.; Leicester COVID-19 consortium. Socio-demographic heterogeneity in the prevalence of COVID-19 during lockdown is associated with ethnicity and household size: Results from an observational cohort study. EClinicalMedicine. 2020;25:
100466 . DOIPubMedGoogle Scholar - Endo A, Abbott S, Kucharski AJ, Funk S; Centre for the Mathematical Modelling of Infectious Diseases COVID-19 Working Group. Estimating the overdispersion in COVID-19 transmission using outbreak sizes outside China. Wellcome Open Res. 2020;5:67. DOIPubMedGoogle Scholar
- Leng T, Hill EM, Holmes A, Southall E, Thompson RN, Tildesley MJ, et al. Quantifying pupil-to-pupil SARS-CoV-2 transmission and the impact of lateral flow testing in English secondary schools. Nat Commun. 2022;13:1106. DOIPubMedGoogle Scholar
- Woody S, Javan E, Johnson K, Pasco R, Johnson-León M, Lachmann M, et al. Spatial distribution of COVID-19 infections and vaccinations in Austin, Texas. University of Texas at Austin. 2021 [cited 2021 Jul 5]. https://covid-19.tacc.utexas.edu/media/filer_public/fe/f2/fef289f8-800c-4390-ab27-6eff3b229f59/covid_infections_and_vaccinations_-_austin_zip_codes_-_ut_-_041221.pdf
Figures
Table
Cite This ArticleOriginal Publication Date: January 26, 2023
Table of Contents – Volume 29, Number 3—March 2023
| EID Search Options |
|---|
|
|
|
|
|
|


Please use the form below to submit correspondence to the authors or contact them at the following address:
Lauren Ancel Meyers, Department of Integrative Biology, 1 University Station C0990, Austin, TX 78712, USA
Top