Food Poisoning from Marine Toxins
CDC Yellow Book 2024
Environmental Hazards & RisksPoisoning from ingesting marine toxins is an underrecognized hazard for travelers, particularly in the tropics and subtropics. Climate change, coral reef damage, expanding international trade and tourism, growing seafood consumption, and spread of toxic algal blooms are all contributing to an increasing risk (Map 4-01).
Map 4-01: Worldwide distribution of selected seafood poisonings
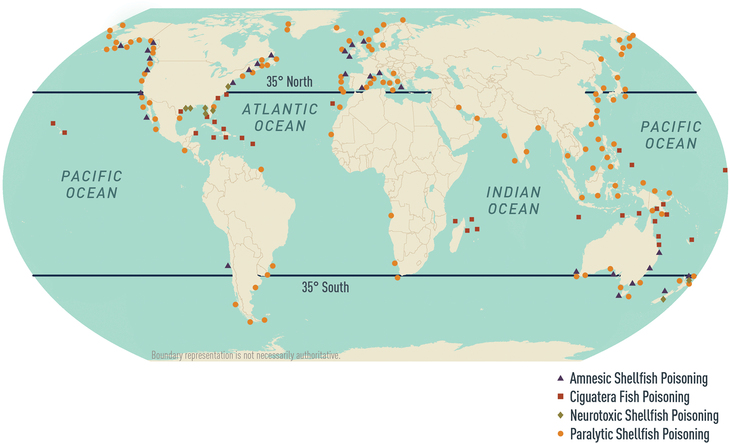
Source: US National Office for Harmful Algal Blooms, Woods Hole Oceanographic Institution, Woods Hole, MA: 2016. Available from: https://hab.whoi.edu/maps/regions-world-distribution/. Harmful algal blooms (HABs) occur widely and contribute to seafood toxicity. Risk for human poisoning depends on the particular seafood consumed, where it was caught or harvested, and—in some instances—the exposure of that seafood to an HAB.
Ciguatera Fish Poisoning
Ciguatera fish poisoning occurs after eating reef fish contaminated with toxins like ciguatoxin or maitotoxin. These potent toxins originate from Gambierdiscus toxicus, a small marine organism (dinoflagellate) that grows on and around coral reefs. Dinoflagellates are ingested by herbivorous fish. The toxins produced by G. toxicus are then modified and concentrated as they pass up the marine food chain to carnivorous fish and finally to humans. Ciguatoxins are concentrated in fish liver, intestines, roe, and heads.
G. toxicus might proliferate on dead coral reefs more effectively than other dinoflagellates. The risk for ciguatera poisoning is likely to increase as coral reefs deteriorate because of climate change, ocean acidification, offshore construction, and nutrient runoff.
Risk to Travelers
Approximately 50,000 cases of ciguatera poisoning are reported worldwide annually, but because the disease is underrecognized and underreported, reports are likely grossly underestimated. The incidence in travelers to highly endemic areas has been estimated as high as 3 per 100. Ciguatera is widespread in tropical and subtropical waters, usually between the latitudes of 35°N and 35°S, and is particularly common in the Pacific and Indian Oceans and the Caribbean Sea. The incidence and geographic distribution of ciguatera poisoning are increasing. Newly recognized areas of risk include Madeira and the Canary Islands, parts of the Mediterranean, and the western Gulf of Mexico. Be aware that travelers with ciguatera fish poisoning might seek care after returning home to nonendemic (temperate) areas. In addition, cases of ciguatera fish poisoning are seen with increasing frequency in nonendemic areas because of the increasing global trade in seafood products.
Fish most likely to cause ciguatera poisoning are large carnivorous reef fish (e.g., amberjack, barracuda, grouper, moray eel, sea bass, sturgeon). Omnivorous and herbivorous fish (e.g., parrot fish, red snapper, surgeonfish) also can be a risk.
Clinical Presentation
Ciguatera poisoning can cause cardiovascular, gastrointestinal, neurologic, and neuropsychiatric illness. The first symptoms usually develop within 3–6 hours after eating contaminated fish but can be delayed up to 30 hours. General signs and symptoms include fatigue, general malaise, and insomnia. Cardiovascular signs and symptoms include bradycardia, heart block, or hypotension. Gastrointestinal signs and symptoms include diarrhea, nausea, vomiting, and abdominal pain. Neurologic and neuropsychiatric signs and symptoms include paresthesia, weakness, pain in the teeth or a sensation that the teeth are loose, a burning or metallic taste in the mouth, generalized itching, sweating, and blurred vision. Cold allodynia (abnormal sensation when touching cold water or objects) has been a reported characteristic, but acute sensitivity to both heat and cold can be present. Neurologic symptoms usually last a few days to several weeks but can persist for months or even years.
The overall death rate from ciguatera poisoning is <0.1% but varies according to the toxin dose and availability of medical care to deal with complications. The diagnosis of ciguatera poisoning is based on the characteristic signs and symptoms and a history of eating fish species known to carry ciguatera toxin. The US Food and Drug Administration (FDA) can test fish in their laboratory at Dauphin Island, Alabama. No test for ciguatera toxins in human clinical specimens is readily available.
Prevention
Ciguatera toxins do not affect the texture, taste, or smell of fish, nor are they destroyed by canning, cooking, freezing, pickling, salting, or smoking, or by gastric acid. To prevent ciguatera fish poisoning, travelers should avoid or limit consumption of reef fish, particularly fish that weigh >5 pounds; counsel travelers to never eat high-risk fish (e.g., barracuda, moray eel) and to avoid eating the parts of the fish (e.g., the head, intestines, liver, roe) that concentrate ciguatera toxin.
Treatment
No specific antidote for ciguatoxin or maitotoxin poisoning is available. Symptomatic treatments include amitriptyline for chronic paresthesias, depression, or pruritus; fluoxetine for chronic fatigue; gabapentin or pregabalin for neuropathic symptoms; and nifedipine or acetaminophen for headaches. Intravenous mannitol has been reported in uncontrolled studies to reduce the severity and duration of neurologic symptoms, particularly if given ≤48 hours of symptom onset; give mannitol only to hemodynamically stable, well-hydrated patients.
After recovery, advise patients to avoid consuming alcohol, caffeine, fish, and nuts for ≥6 months because these might cause symptom relapse.
Scombroid
Scombroid is caused by eating fish that contain high levels of histamine. Bacteria convert histidine, an essential amino acid found in the flesh of the fish, to histamine. The process of histidine conversion can be mitigated by inhibiting bacterial growth through proper storage of freshly caught fish by refrigeration or icing. Conversely, when fish are improperly stored after capture, bacterial overgrowth can occur, facilitating and accelerating histamine production.
One of the most common fish poisonings, scombroid occurs worldwide in both temperate and tropical waters. Fish typically associated with scombroid have naturally high levels of histidine in their flesh and include amberjack, anchovies, bluefish, herring, mackerel, mahi mahi (dolphin fish), marlin, sardines, and tuna. Histamine and other scombrotoxins are resistant to canning, cooking, freezing, and smoking.
Clinical Presentation
Scombroid poisoning resembles an acute allergic reaction and usually appears 10–60 minutes after a person eats contaminated fish. Signs and symptoms include abdominal cramps and diarrhea, blurred vision, flushing of the face and upper body resembling sunburn, severe headaches, itching, and palpitations. Left untreated, symptoms usually resolve within 12 hours but can last ≤48 hours.
Rarely, respiratory compromise, malignant arrhythmias, and hypotension requiring hospitalization can occur. Scombroid poisoning has no long-term sequelae and usually is diagnosed from clinical signs and symptoms. Clustering of cases helps exclude the possibility of true fish allergy.
Prevention
Fish contaminated with histamine can have a peppery, sharp, or salty taste or a “bubbly” feel, but will usually look, smell, and taste normal. The key to prevention is to make sure fish are properly iced or refrigerated at temperatures <38°F (<3.3°C) or immediately frozen after being caught. Canning, cooking, freezing, or smoking will not destroy histamine in contaminated fish.
Treatment
Scombroid poisoning usually responds well to antihistamines, typically H1-receptor antagonists, although H2-receptor antagonists also might provide some benefit.
Shellfish Poisoning
Shellfish, including crustaceans (Dungeness crab, lobster, and shrimp), filter-feeding bivalve mollusks (clams, cockles, mussels, oysters, and scallops), and gastropod mollusks (abalone, moon snails, and whelks) can harbor toxins that result in several different poisoning syndromes. Toxins originate in small marine organisms (diatoms or dinoflagellates) ingested and concentrated by shellfish.
Risk to Travelers
Contaminated (toxic) shellfish can be found in temperate and tropical waters, typically during or after phytoplankton blooms, also called harmful algal blooms (HABs). One example of a HAB is the Florida red tide caused by Karenia brevis.
Clinical Presentation
Poisoning results in gastrointestinal and neurologic illness of varying severity. Symptoms typically appear 30–60 minutes after a person ingests toxic shellfish but can be delayed for several hours. Diagnosis is usually through exclusion, and typically is made clinically in patients with a history of having recently eaten shellfish.
Amnesic Shellfish Poisoning
Amnesic shellfish poisoning (ASP) is a rare form of shellfish poisoning caused by eating shellfish contaminated with domoic acid, produced by diatoms of the Pseudonitzchia spp. Outbreaks of ASP have been reported in the Americas (Canada, Chile), Europe (Belgium, France, Ireland, Portugal, Scotland, Spain), and the Pacific (Australia, New Zealand). Implicated shellfish include razor clams, mussels, scallops, and other crustaceans.
In most cases, gastrointestinal symptoms (e.g., abdominal pain, diarrhea, vomiting) develop within 24 hours of eating toxic shellfish, followed by headache, cognitive impairment, and memory loss. Symptoms usually resolve within hours to days after shellfish ingestion. Hypotension, arrhythmias, ophthalmoplegia, coma, and death have been reported in severe cases. Survivors might exhibit severe anterograde, short-term memory deficits.
Diarrheic Shellfish Poisoning
Diarrheic shellfish poisoning (DSP) results from eating shellfish contaminated with toxins (e.g., okadaic acid). DSP occurs worldwide, and outbreaks have been reported in the Americas (Canada, Chile, United States, and Uruguay), Asia (China, Japan), and Europe (Belgium, France, Ireland, Scandinavia, Spain).
Most cases result from eating toxin-containing bivalve mollusks (e.g., mussels, scallops). Symptoms usually occur within 2 hours of consumption and include abdominal pain, chills, diarrhea, nausea, and vomiting. Symptoms usually resolve within 2–3 days. No deaths from DSP have been reported.
Neurotoxic Shellfish Poisoning
Neurotoxic shellfish poisoning (NSP) is caused by eating shellfish contaminated with brevetoxins produced by the dinoflagellate K. brevis. NSP is predominately an illness of the Western Hemisphere (the Caribbean, Gulf of Mexico, southeastern coast of the United States), but the disease also has been reported from New Zealand.
NSP usually presents as a gastroenteritis accompanied by neurologic symptoms resembling mild ciguatera or paralytic shellfish poisoning (described below), 30 minutes to 3 hours after a person eats shellfish. Aerosolized red tide respiratory irritation (ARTRI) also can occur when people inhale aerosolized brevetoxins in sea spray, and has been reported in association with a red tide (K. brevis HAB) in Florida. ARTRI can induce bronchoconstriction and cause acute, temporary respiratory discomfort in healthy people. People with asthma might experience more severe and prolonged respiratory effects.
Paralytic Shellfish Poisoning
Paralytic shellfish poisoning (PSP) is the most common and most severe form of shellfish poisoning. PSP is caused by eating shellfish contaminated with saxitoxins. These potent neurotoxins are produced by various dinoflagellates. A wide range of shellfish can cause PSP, but most cases occur after people eat clams or mussels.
PSP occurs worldwide but is most common in temperate waters off the Atlantic and Pacific coasts of North America, including Alaska. Other countries in the Americas (Chile), as well as countries in Asia (China, the Philippines), Europe (Ireland, Scotland), and the Pacific (Australia, New Zealand) have also reported cases.
Symptoms usually appear 30–60 minutes after a person eats toxic shellfish and include numbness and tingling of the face, lips, tongue, arms, and legs. Patients also might have diarrhea and vomiting, headache, and nausea. Severe cases are associated with ingestion of large doses of toxin and clinical features such as ataxia, dysphagia, flaccid paralysis, mental status changes, and respiratory failure. The case-fatality ratio depends on the availability of modern medical care, including mechanical ventilation; rates of death among children can be particularly high.
Prevention
Shellfish poisoning can be prevented by avoiding potentially contaminated shellfish, which is particularly important in areas during or shortly after algal blooms, locally referred to as “red tides” or “brown tides.” Consuming shellfish also carries a very high risk for infection from various viral (e.g., hepatitis A virus, norovirus) and bacterial (e.g., Salmonella, Shigella, Vibrio parahaemolyticus, and V. vulnificus) pathogens. Ideally, travelers to developing countries should consider avoiding eating shellfish. Marine shellfish toxins cannot be destroyed by cooking or freezing.
Treatment
Treatment is symptomatic and supportive. Severe cases of paralytic shellfish poisoning might require mechanical ventilation.
The following authors contributed to the previous version of this chapter: Vernon E. Ansdell