Humanitarian Aid Workers
CDC Yellow Book 2024
Travel for Work & Other ReasonsHumanitarian aid workers assist people forced from their homes because of conflict or natural disasters. Assistance begins within hours after a disaster and often continues for years. Humanitarian relief deployments can last for weeks to years; the work can be rewarding and adventurous but requires preparation. During deployments, humanitarian aid workers must plan to be self-sufficient and to face unique challenges, including insecure environments and emotional stress.
Each year hundreds of thousands of professional aid workers are deployed worldwide to support people affected by disaster and conflict. Many of these efforts are coordinated by the United Nations Office for the Coordination of Humanitarian Affairs, whose appeals in 2021 identified 235 million people in 34 countries or regions in need, a number that continues to grow (Figure 9-01).
Professional aid workers often deploy with large specialist organizations (e.g., Doctors Without Borders) that have infrastructure and resources to properly support their personnel. Many more people (e.g., doctors, civic and religious groups) participate as amateur responders to international disasters. In contrast with professional aid workers, amateur responders might deploy with smaller, less prepared groups and little experience in providing humanitarian aid (Box 9-05).
Figure 9-01 Trends in the global number of people in need of humanitarian assistance (2015–2022)
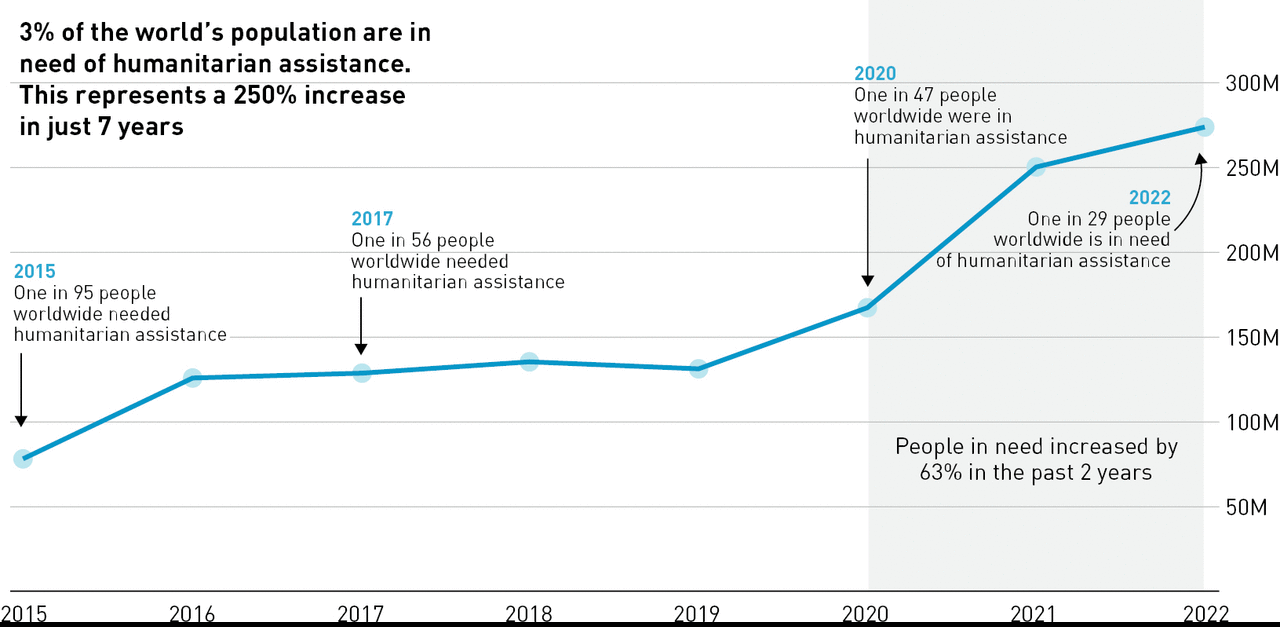
Source: Global Humanitarian Overview 2022. United Nations Office for the Coordination of Humanitarian Affairs. Inter-Agency Coordinated Appeals: Overview for 2022. Available from: https://gho.unocha.org/appeals/inter-agency-coordinated-appeals-overview-2022.
Box 9-05 Voluntourism
Volunteer tourism (also called “voluntourism”) describes tourists volunteering for a charity or development organization, usually for short periods, in low- and middle-income countries. Although largely well intentioned, the impact of short-term visits—often by volunteers lacking specific understanding of the local context and lacking requisite training or skills—is variable and might be harmful in certain settings.
Voluntourism in humanitarian emergencies can be particularly problematic given dynamic and often dangerous humanitarian environments that require professional knowledge, organizational infrastructure, and understanding of the humanitarian response coordination system. Without the necessary individual competencies and organizational support, voluntourists in these settings expose themselves to unnecessary personal risks and can create a burden on the broader humanitarian response operations.
Unique Challenges
Aid workers experience situations and specific risks (e.g., safety, security, mental health) related to providing humanitarian relief. Safety and security challenges include exposure to the conflict or disaster environment that precipitated or sustained the crisis; damaged or absent infrastructure (e.g., living accommodations, sanitation facilities); and high levels of insecurity. Mental health risks include living in stressful environments; working long hours under adverse or extreme conditions; and challenges to reentering home life and postdeployment activities.
Humanitarian service can have an adverse effect on personal health. Studies of long-term humanitarian aid workers indicate that >35% report a deterioration in their personal health during the mission. Injuries from accidents and violence are risks for humanitarian aid workers and cause more deaths than disease or natural causes. Recent estimates place the risk for medical evacuations, hospitalizations, and violence-related deaths at ≈6 per 10,000 person-years among aid workers. Conditions and outcomes vary by location, nature of the humanitarian event, and time spent in the field. A study of American Red Cross workers reported that 10% experienced accident or injury and 16% were exposed to violence. The same study demonstrated that >40% found the experience more stressful than expected.
Safety & Security
Security risks and targeting of aid workers with kidnapping and violence continues to be a concern for the humanitarian community. Risks to staff are not uniformly distributed across the humanitarian landscape, however. Ongoing surveillance of violence directed against humanitarian aid and disaster relief workers continues to demonstrate that most of these events occur in a few insecure locations, including Afghanistan, Cameroon, Central African Republic, Democratic Republic of the Congo, Ethiopia, Mali, Nigeria, Somalia, South Sudan, and Syria.
Injuries and motor vehicle accidents are common risks for travelers, including humanitarian aid workers, throughout the world. Aid workers should be sensitive to their surroundings and carefully select the type of transportation and hour of travel, if possible (see Sec. 8, Ch. 5, Road & Traffic Safety).
In disaster and emergency situations, aid workers should be aware of physical hazards (e.g., debris, downed power lines, unstable structures, and other environmental hazards). Workers in certain conflict and post-conflict settings should be educated on improvised explosive devices, landmines, and other unexploded ordnance. Although less common, some environments might involve unusual exposures, such as radiation (e.g., after the 2011 earthquake and tsunami in Japan) or chemical agents (e.g., mustard gas and sarin used on civilians in the Syrian conflict). Humanitarian aid and disaster relief workers who will be deployed to insecure areas, including active conflict zones, should undergo specialized security briefings by the deploying agency or private sources. Reputable and free resources exist for basic security training (e.g., the United Nations BSAFE course).
In situations associated with damage or destruction to local services and facilities, humanitarian aid workers should anticipate and plan for limited accommodations and logistical and personal support. Humanitarian aid and disaster relief workers destined for low-resource areas or situations can benefit from pretravel training and counseling regarding the moral complexities of providing service in these environments.
Encourage humanitarian aid workers from the United States to enroll in the Department of State’s Smart Traveler Enrollment Program (STEP) to register with the US embassy in their destination country. Enrollment before departure will ensure that the local consulate is aware of their presence and can provide them with notifications, account for them, and include them in evacuation plans.
Travelers providing humanitarian assistance should review and understand medical, evacuation, and life insurance provided by their employing agency. They also should consider supplemental travel, travel health, and medical evacuation insurance to cover medical care and evacuation should they become ill or injured (see Sec. 6, Ch. 1, Travel Insurance, Travel Health Insurance & Medical Evacuation Insurance). Travelers should carefully review evacuation policies for any exclusions, such as from higher risk countries or potential exposure to certain infectious diseases (e.g., Ebola, coronavirus disease 2019 [COVID-19]).
Mental Health
Studies suggest that aid workers returning from humanitarian missions, particularly missions characterized by high or chronic stress, have increased symptoms of anxiety, depression, and posttraumatic stress disorder. People with preexisting mental health issues, including anxiety and depression, could be predisposed to worse outcomes.
Generally, humanitarian aid and disaster relief workers demonstrate considerable resilience and adapt to the stressful environments, but elevated and chronic stress can lead to deterioration in mental health and decompensation in some people. Predeployment briefings can increase an aid worker’s ability to cope with highly stressful environments; data are lacking, however, on the effectiveness of postdeployment debriefings to decrease adverse mental health impacts of deployment.
A detailed evaluation of risk factors (e.g., preexisting mental illness, family history of mental illness, history of alcohol or substance use disorder) might identify previously unrecognized chronic mental health conditions. Identifying alcohol or substance dependence or underlying mental health issues (e.g., depression) is particularly important because stressful humanitarian environments frequently exacerbate these conditions, which are often the reason for emergency repatriation (see Sec. 2, Ch. 12, Mental Health, and Sec 3, Ch. 5, Substance Use & Substance Use Disorders).
Preparation
Careful attention to pretravel evaluation, both physical and mental health, can reduce the likelihood of illness and the need for emergency repatriation of humanitarian aid workers. Comprehensive medical and—for those planning long-term assignments—dental evaluations can prepare aid workers by identifying previously unrecognized conditions, enabling treatment before travel. Medical illness or injury among deployed staff, particularly serious conditions that require repatriation, are not only burdensome and potentially dangerous for the affected staff member, but these events redirect limited organizational resources from the intended beneficiaries.
Most of the core elements of the pretravel evaluation and counseling are discussed in detail in Sec. 2, Ch. 1, The Pretravel Consultation, and in Sec. 9, Ch. 4, Health Care Workers, Including Public Health Researchers & Medical Laboratorians. Administer routine vaccinations and prescribe malaria prophylaxis or medications to prevent altitude sickness, as appropriate. COVID-19 risk and related guidance can vary based on the individual and the destination, but the Centers for Disease Control and Prevention recommends vaccination for all travelers. Additional COVID-19 guidance is discussed in Sec. 5, Part 2, Ch. 3, COVID-19. Give guidance on food and water precautions; self-treatment for travelers’ diarrhea; protection from insect bites; environmental protection from the elements including sun exposure; behavioral risk avoidance; and injury prevention. Several of these topics listed here are covered in detail in Section 2 and Section 4.
For health care workers providing medical care as part of their humanitarian activities, evaluate occupational risk and the need for preventive preexposure or postexposure interventions. Medical humanitarian aid workers responding to outbreaks of communicable diseases are often at increased risk for exposure and infection by specific infectious pathogens, which requires meticulous attention to infection control and personal protective measure protocols. Medical workers (see Sec. 9, Ch. 4, Health Care Workers, Including Public Health Researchers & Medical Laboratorians) should ensure their organization provides adequate safety protocols and personal protective equipment (e.g., gloves, gowns, masks, eye protection).
In humanitarian emergencies, direct infrastructure damage; lack of equipment, supplies, and human resources; or a surge in medical need can all contribute to a medical facility becoming compromised or overwhelmed. Counsel volunteers with significant underlying medical conditions, who are likely to require care themselves, against travel; encourage them to support the response in other ways. Similarly, a woman who is pregnant should discuss her plans with their obstetrician and should typically be advised to defer deployment.
For travelers planning to participate in animal rescue activities, share information available in Sec. 4, Ch. 9, Bringing Animals & Animal Products into the United States, and discuss rabies preexposure prophylaxis (see Sec. 5, Part 2, Ch. 18, Rabies).
Travel Health Kits
In general, because aid workers will need a more comprehensive travel health kit than the typical traveler (Sec. 2, Ch. 10, Travel Health Kits), they should consult with their deploying organization to determine how extensively to tailor their packed supplies. For example, health care workers deployed by a medical organization will usually be able to access basic pharmacologic and other medical supplies for acute care treatment from the organization and should be familiar with basic first aid to self-treat any injury until they can obtain medical attention.
Conversely, people with chronic medical conditions requiring treatment should ensure they travel with prescriptions and medications sufficient for the duration of their service. They also should consider bringing along treatment for exacerbations of diseases or conditions they might not usually experience (e.g., asthma, back pain). Because not all pharmaceuticals are globally available, travelers on extended deployments should review safe alternatives to their regular medication (see Sec. 6, Ch. 3, . . . perspectives: Avoiding Poorly Regulated Medicines & Medical Products During Travel). Aid workers should store medications in 2 separate allotments in case of loss or theft. Sec. 2, Ch. 10, Travel Health Kits, provides additional information on preparing, storing, and traveling with medications.
People with dental crowns or bridgework should consider taking temporary dental adhesive for short-term management of a dislodged dental appliance. In addition to a basic travel health kit, humanitarian aid workers should consider bringing the items listed in Box 9-06.
Box 9-06 International humanitarian aid travel health kit checklist: additional items
☐ Cash (new or crisp bills can often be exchanged at better rates)
☐ Contact lenses, prescription glasses (extra pairs, if applicable)
☐ Gloves (leather gloves if physical labor will be performed)
☐ Headlamp and spare batteries
☐ Insect repellent
☐ Insecticide-impregnated mosquito net (if traveling to areas endemic for insect-borne diseases)
☐ Long pants, shirts that cover the shoulders
☐ Menstrual supplies
☐ Mobile telephone, equipped to work internationally (or preferably unlocked)
☐ Money belt
☐ Safety goggles
☐ Sewing kit
☐ Sturdy work boots (particularly in disaster or rudimentary settings)
☐ Sunglasses
☐ Sunscreen
Personal Items
Loss of life, serious injuries, missing and separated families, and destruction of communities are often associated with humanitarian emergencies; aid workers should recognize they are likely to encounter stressful situations as part of their work. Keeping a personal item nearby (e.g., a family photo, favorite music, religious or spiritual material) can offer comfort. Communicating with family members and close friends from time to time can be an important means of support.
Access to mobile phones and internet services are frequent challenges in humanitarian emergencies. Global mobile coverage continues to improve, however, and free applications (e.g., WhatsApp) have expanded accessibility. For more remote regions, satellite telephones are an option, although some government authorities might prohibit or limit their importation and use, particularly in conflict zones. Before travel, aid workers should clarify any restrictions to telephone, internet, or satellite technology in the destination country.
Documents
Aid workers should carry extra passport-style photos, which might be required for certain types of security passes, visas, and work permits. Travelers should bring photocopies of documents (e.g., credit cards, passports) and copies of their medical, nursing, or other professional licenses, if applicable.
Aid workers also should have medical information (e.g., blood type, immunization records), available. Travelers should carry physical copies of all these documents, leave copies with their main contact at home, scan and email copies to their smartphones (if appropriate), and ensure the documents are securely stored and available in a cloud storage service. In addition, aid workers should carry information for their emergency contacts written on paper, and not rely exclusively on an electronic device.
Posttravel
Returning humanitarian aid and disaster relief workers should seek medical care if they sustained injuries during their travel or become ill after returning home. To ensure a thorough assessment, returning aid workers should advise their providers of the nature and location of their recent travel. Depending on the duration and nature of the deployment, including if they were providing direct medical care, returning aid workers might benefit from a comprehensive medical review. Educate workers involved in responding to infectious disease outbreaks on posttravel illness monitoring recommendations or requirements, if applicable.
Homecoming can be psychologically challenging, and aid workers should seek treatment or counseling if they have concerns about transitioning to postdeployment life. Consider referring workers who witnessed or were involved in mass casualties, deaths, or serious injuries or who have been victims of violence (e.g., assault, kidnapping, serious road traffic crash) for critical incident counseling. Educate returning aid workers that the onset of adverse psychological effects after exposure to traumatic experiences can be delayed, sometimes by several months or longer.
The following authors contributed to the previous version of this chapter: Eric J. Nilles, Brian D. Gushulak, Stephanie Kayden